What is a bursa you ask? A bursa is small fluid sack located between muscle, tendon, bone and the skin. These fluid sacs function to cushion the joint and minimise the friction and irritation that can occur between these tissues when they move. Most of the time these fluid sacs are not painful and aid in improving movement of the shoulder.
Shoulder bursitis is, therefore, when the bursa sac becomes inflamed, swollen and irritated within the confines of the shoulder bones (called your scapula, humerus and clavicle). Generally, people present with pain on the front and outside of the shoulder and they explain how the pain feels very deep in the joint. Most people have a history of trauma (like a fall), pain with reaching movements, lifting overhead, lifting their arm out to the side and often have pain at night which interrupts their sleep. We have already seen an increase of this condition presenting at OHL with more people working from home in ‘less than ideal ergonomic set ups’.
Recent studies and medical researchers have found that shoulder bursitis generally does not occur alone and it usually associated trauma and/or loss of function such as muscle weakness, so we need to fully evaluate your shoulder joint and related structures to best understand your pain sources. Other conditions which can also cause irritation to your shoulder bursa include shoulder instability, rotator cuff tears, poor scapula muscle control and/or osteoarthritis of the glenohumeral joint or AC joint.
Our team of physiotherapists are highly trained to take you through a thorough assessment of the shoulder joint using muscle strength, palpation and special tests to establish the cause and type of injury that has occurred to the shoulder joint. This assessment allows us to best establish a plan for treatment based off each patients individual needs and injuries.
The most common treatment of shoulder bursitis sees the Physio focus on addressing the initial cause of the irritation (as found in their assessment) and potentially address any environmental issues like a poor desk set up forcing you to reach to your computer awkwardly. For example: if the shoulder bursitis is as a result of a rotator cuff tendinopathy or shoulder instability an OHL physiotherapist will initially aid in improving pain, as well as concurrently strengthening any weakened muscles or thickened tendons in the shoulder complex. This will be done through some hands on therapy, but it also often includes a home exercise program, gym program or in our group physiotherapy classes. Most exercises will start gently by your side with minimal weight before progressing you through your range to overhead with weights and theraBand’s once pain and symptoms allow.
Sometimes, as guided by your trusty GP, anti-inflammatory medications can be useful in the early stages to help reduce swelling and pain associated with the injury. Your GP and or pharmacist will best guide you through these medications if they are required.
If pain persists ultrasound guided, corticosteroid injections can be used to reduce pain and symptoms, however as we know that bursitis does not occur alone the underlying cause must then be immediately addressed and treated as guided by your physiotherapist to ensure further irritation does not occur and to reduce symptoms in the long term.
If you or someone you know is suffering from shoulder pain of any type or suspects they have shoulder bursitis come and see our team of physiotherapists so that they can do a thorough assessment, diagnosis and treatment to restore your strength, reduce your pain and get you back to living at your optimal level of health.
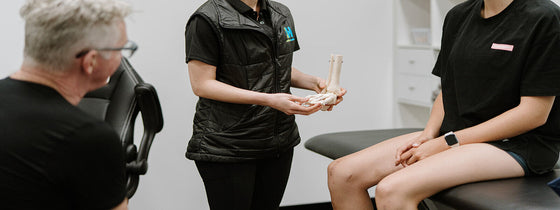
If you're experiencing back or neck pain with neurological signs and symptoms, a thorough neurological examination is crucial for accurate assessment and effective treatment. In this Optimal Tip learn more about what we mean by completing a neurological exam!

Squats, deadlifts, and calf raises are key movement patterns that should be part of every strength and conditioning program—regardless of age and activity level. These functional movements support joint health, improve posture and balance, and reduce the risk of injury while building strength where it matters most.
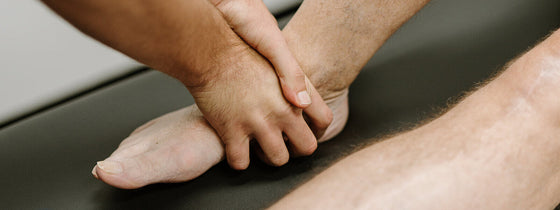
A ganglion cyst is a fluid-filled swelling that typically forms over a joint or tendon sheath, causing discomfort and pain, especially when pressing against nerves or joints. Proper assessment and treatment, including physiotherapy, are essential for managing symptoms and improving function in the presence of a ganglion in your hand, foot, or wrist.